Rightway Healthcare
Medical Concierge / PBM
Company
Rightway Healthcare
Product
PBM
Approach
Desktop
Framework
React/JS
Platform
Web
From Confusion to Clarity: A Guided Pharmacy Benefit Experience
Pain Points
- Members faced confusion comparing complex drug pricing and plan options.
- Lack of transparency made it hard to understand pharmacy vs. mail-order costs.
- Switching to generics wasn’t obvious, leading to higher out-of-pocket costs.
- Open enrollment support depended heavily on health guide expertise — inexperienced guides often had to reschedule calls, which meant:
Reopening the scheduling system
Finding a new slot on the member’s calendar
Creating a new support ticket
Delaying resolution and frustrating both member and guide
Key Features
AI-Assisted Plan Comparison: Automatically analyzes claims history and medication data to recommend the most cost-effective plan and pharmacy options.
Dual Experience Modes:
Fast Track — Quick, AI-driven recommendation for members who prefer immediate answers.
Guided Mode — Step-by-step walkthrough for members who want to explore details and compare options.
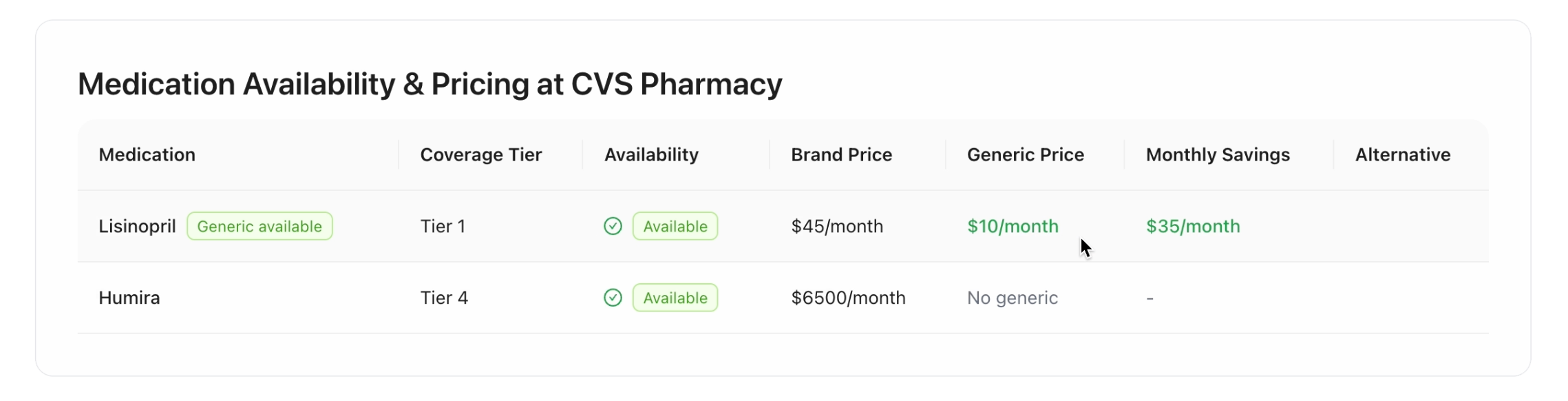
Generic Switch Visibility: Clear monthly savings displayed when switching to generics, improving cost transparency.
Pre-Filled Data: Pulls from historical claims to minimize manual entry and save member time.
Health Guide Support: AI tooltips and recommendations empower less experienced health guides to handle open enrollment calls without rescheduling.
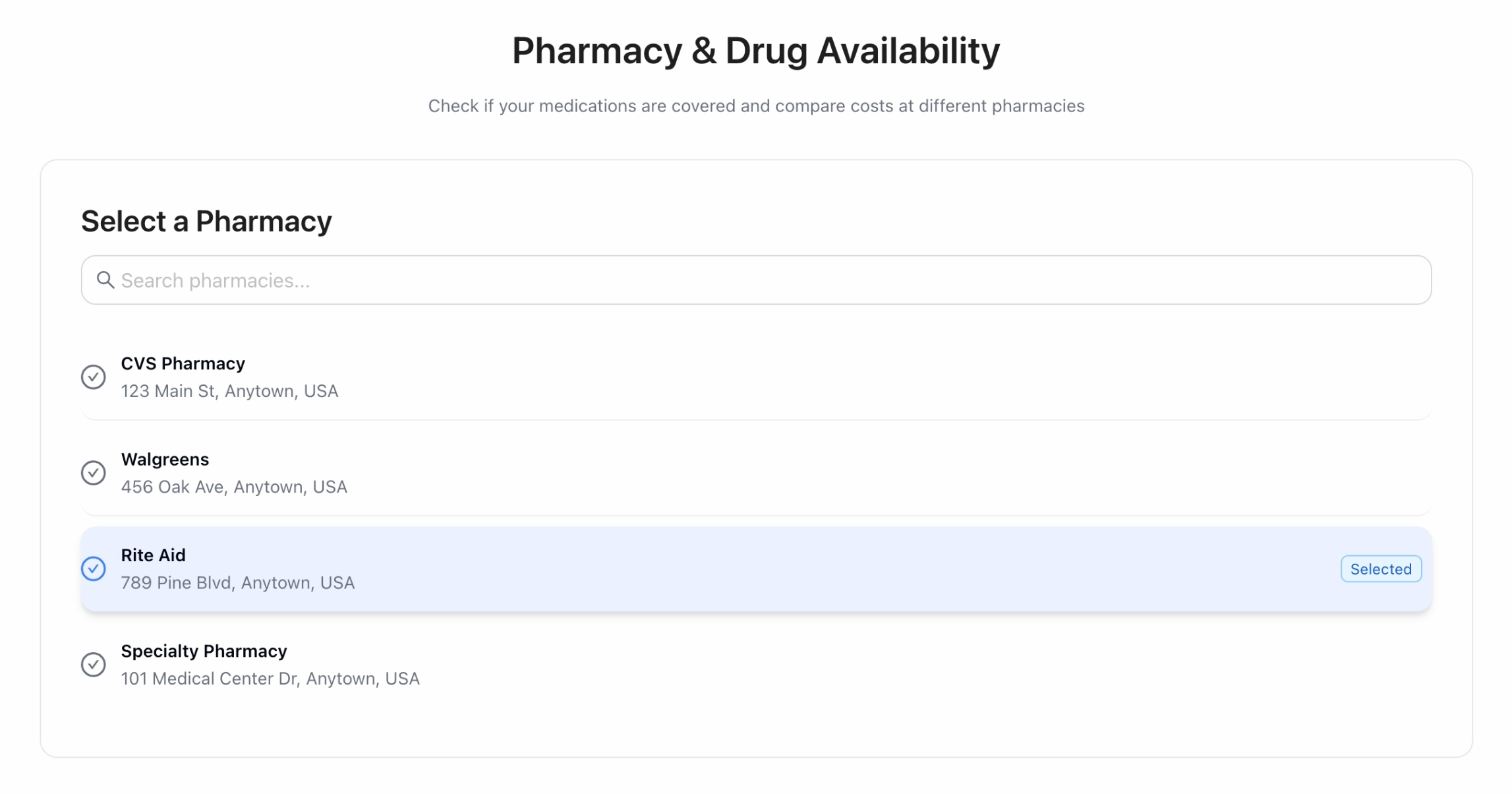
Seamless Pharmacy Options: Side-by-side comparison of retail vs. mail order to maximize convenience and cost savings.
Plan Confirmation Flow: Clear, simple steps to review, confirm, and lock in a plan — reducing errors and decision fatigue.
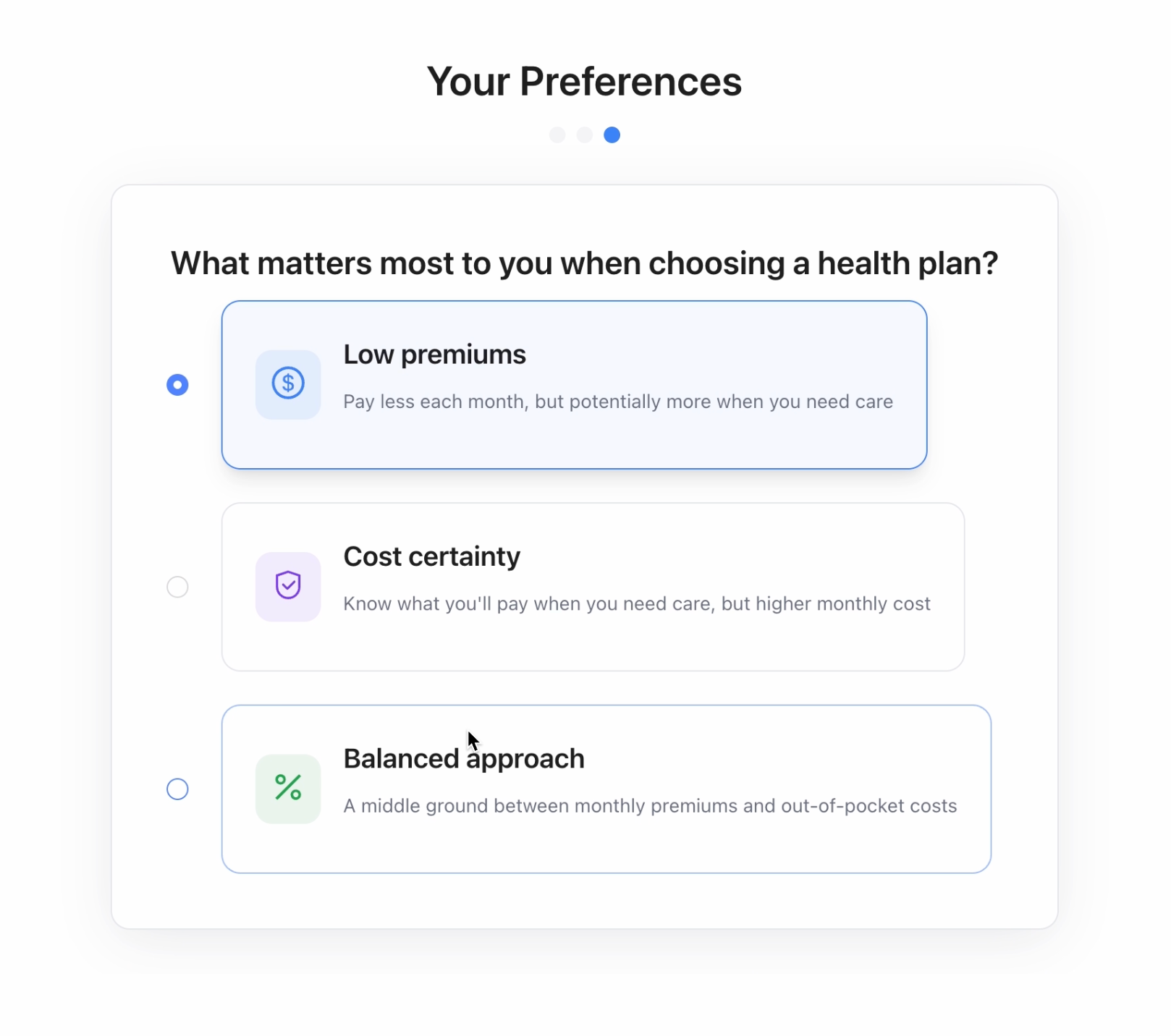
New Design
I redesigned the experience into a guided, AI-assisted plan advisor that consolidates pharmacy benefit data, insurance options, and personal medication history into a single, member-friendly flow.
The new flow was simplified into 3 steps:
- Review Current Plan & Medications (pre-filled with claims data).
- Compare Recommended vs. Available Plans, with AI-driven cost projections and savings opportunities.
- Confirm Plan Selection, with a transparent summary of why the recommendation was made.
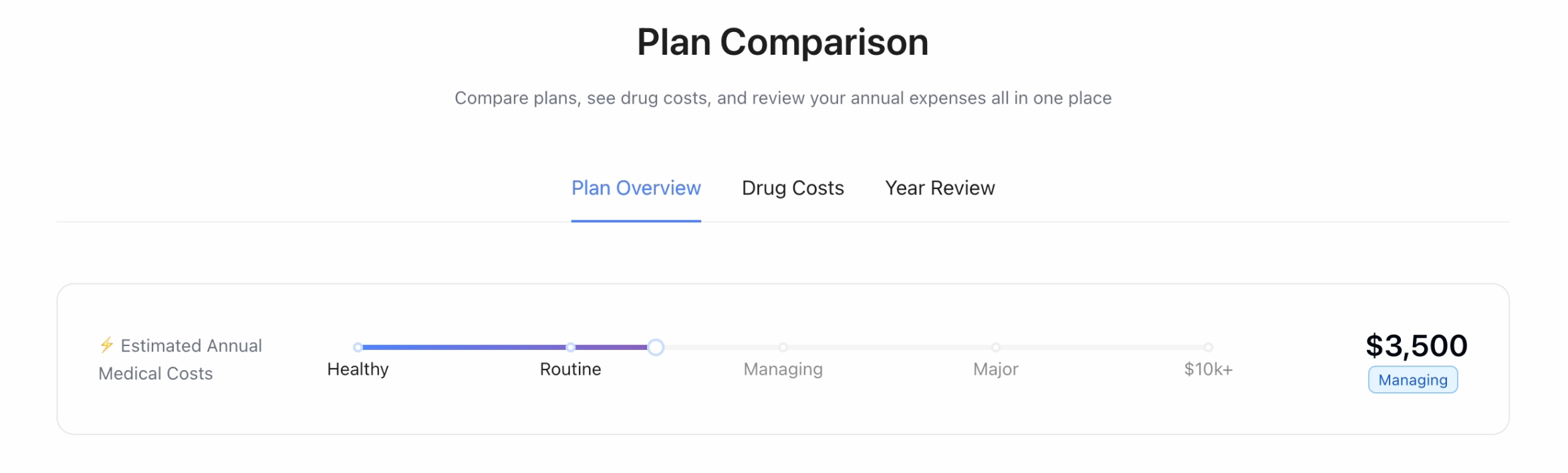
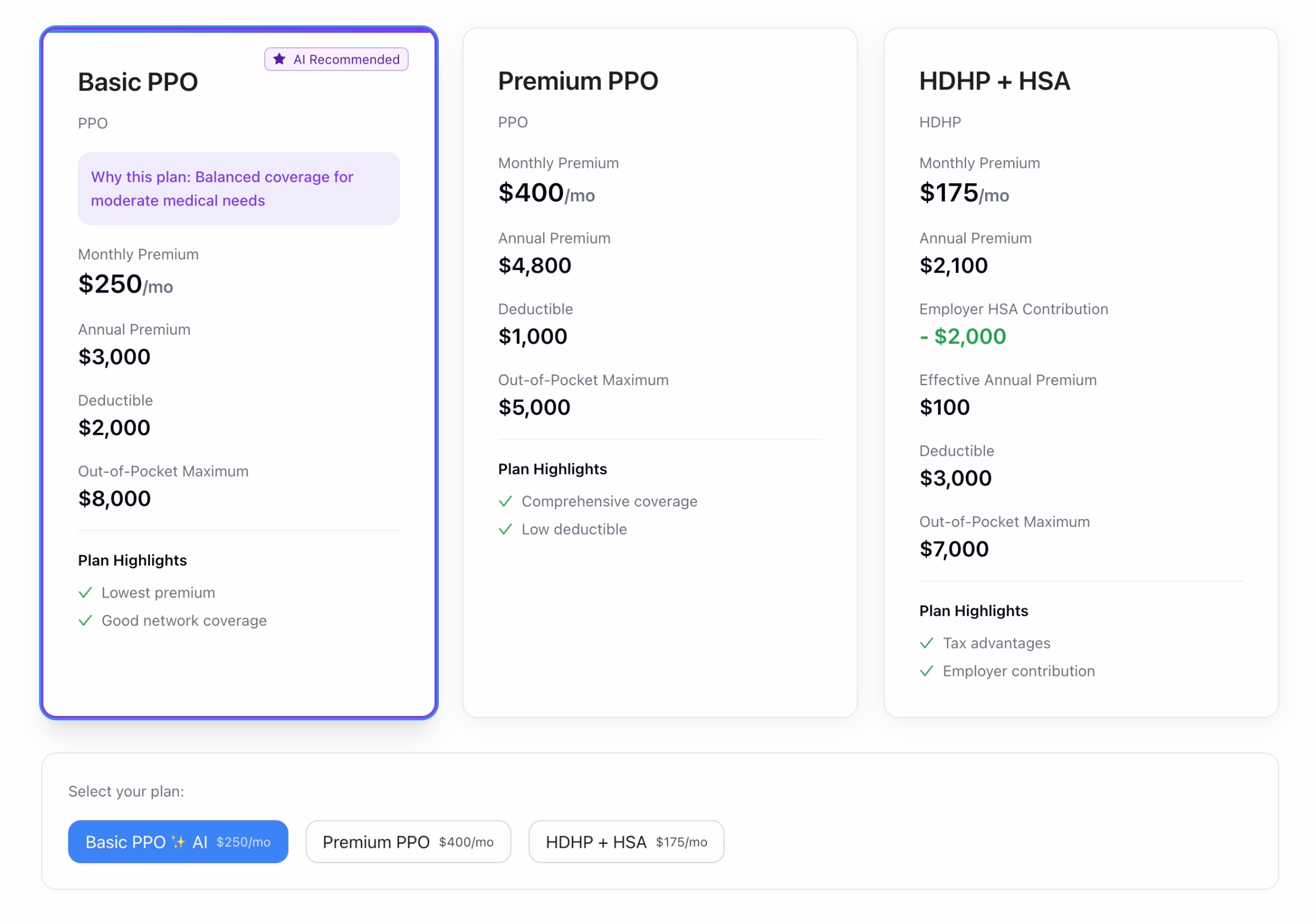
The Impact
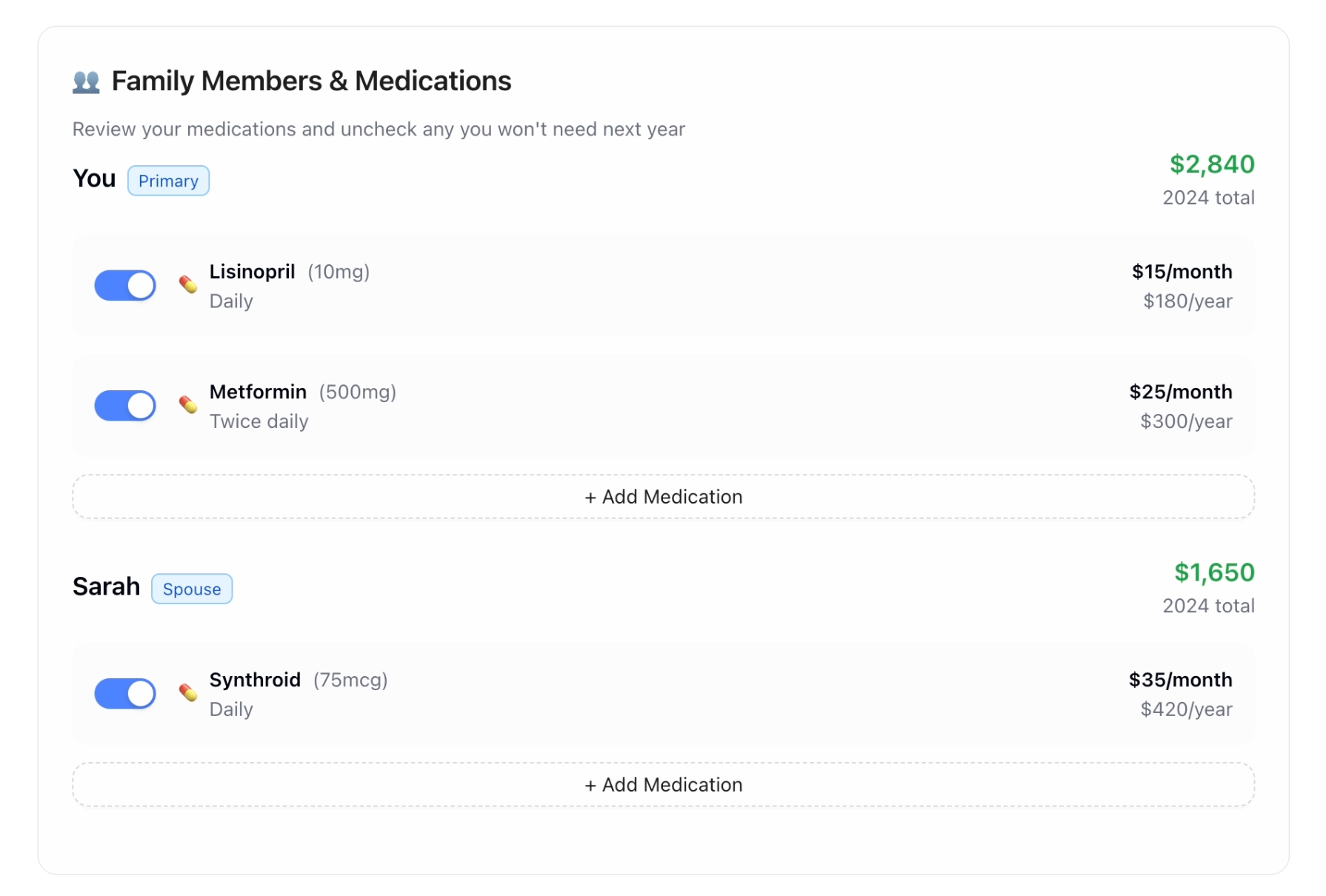
AI assistance reduced dependency on expert guides: Now, even less experienced health guides can use AI-powered plan recommendations during the same call, instead of rescheduling.
Faster resolution: Members get answers in one call, eliminating the need to juggle tickets, calendars, and multiple conversations.
Operational efficiency: Reduced rework freed up scheduling and ticketing resources, lowering overall support costs.
Better member satisfaction: No more waiting days for follow-up — decisions happen in real time.